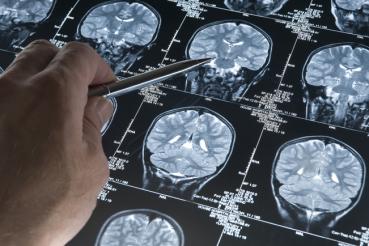
Multiple sclerosis is the ultimate chameleon.
This chronic, inflammatory autoimmune disease affects the central nervous system, resulting in damaged nerves and scar tissue formation, so it can resemble a multitude of other illnesses. This also makes it incredibly hard to detect. And the fact that no two people with MS experience the same symptoms only adds to its unpredictability.
Here's what makes it so tricky: Your brain and spinal cord are full of nerves that send electrical signals rapidly to all areas of your body, which allow you to walk, talk, see, swallow and much more. These nerves are coated in a sheath called myelin that helps transmit the signals.
With MS, the myelin gets destroyed because your immune system mistakenly tells your body to attack it, causing scarring — or sclerosis — and signal interruption. As a result, those with MS experience a variety of different symptoms depending on which signals get interrupted.
"Because MS can develop anywhere within the central nervous system and encompasses the optic nerves, the brain and the spine, a lot of different types of critical attacks can occur, so that leads to diagnostic complexity," says Thomas Shoemaker, MD, a neurologist and MS expert at the Rush Multiple Sclerosis Center.
Although there's currently no cure for MS, there are a number of promising treatments. Being aware of the early symptoms can help you get a diagnosis and start treatment earlier, which can help you better manage the disease. We asked Shoemaker to explain which initial signs to look for, as well as the risk factors associated with the disease.
Here’s where MS (typically) starts
Although a number of MS symptoms can appear early on, two stand out as occurring more often than others:
- Optic neuritis, or inflammation of the optic nerve, is usually the most common, Shoemaker says. You may experience eye pain, blurred vision and headache. It often occurs on one side and can eventually lead to partial or total vision loss.
- Spinal cord inflammation, or what's called partial transverse myelitis, is the second most common symptom Shoemaker typically sees. "You may experience numbness, tingling, weakness in the arms and legs, bladder dysfunction and/or difficulty walking," he explains.
Other early signs of MS include the following:
- Bowel problems range from constipation due to reduced physical activity causing a reduction of food moving through the intestinal tract to diarrhea and incontinence related to neurological dysfunction.
- Depression
- Difficulty thinking
- Fatigue
- Pain, which may be acute or chronic, caused by the nerves that carry sensation "short circuiting." Types of pain can include band-like pain around the chest, or MS hug, caused by spastic nerves along with other types of painful sensations in the neck, arms, legs and feet.
- Sexual problems. These may include changes in sexual function such as arousal and orgasm since arousal starts in the central nervous system and nerve pathways become damaged. MS may also create psychological factors such as mood changes and lower self-esteem that can affect sexual desire as well.
Detecting MS earlier and starting MS therapies earlier tend to improve the chances of having a good long-term outcome.
MS can also look like this
Another potential harbinger of MS is clinically isolated syndrome, or CIS, but this condition is complicated.
"CIS is kind of within the spectrum of MS. In fact, sometimes CIS is just the initial presentation of MS. And people with CIS often will go on to develop multiple sclerosis, but not always," Shoemaker explains.
CIS is basically the first brush with MS, where neurological symptoms occur that often last 24 hours. The episode may result in one symptom or multiple, depending on scarring that occurs in one place or several places. The most common CIS symptoms include the following:
- Optic neuritis
- Numbness
- Slurred speech
- Tingling
- Weakness in legs
If you're experiencing these symptoms, it's important to see a doctor as soon as possible. If testing doesn't reveal a high risk for MS, CIS could signal another serious condition that needs prompt attention, including the following:
- Autoimmune conditions that cause blood vessel inflammation
- Exposure to toxic materials
- Serious vitamin B12 deficiency
- Viral infection
Proper testing shows the bigger picture
Even if you have symptoms associated with MS, you may not have MS. You'll need to confirm the diagnosis.
"No single MS test exists, so the diagnosis can be delayed, incorrect or even missed altogether," Shoemaker says. "An MS diagnosis really requires the synthesis of lots of different types of information by experts who know what to look for and how to put the pieces together."
That's why he recommends seeing a neurologist, who can ensure that the appropriate testing is done to get a complete and accurate picture.
This usually includes having an MRI of the brain and spine, which can reveal changes in the central nervous system that indicate MS.
"You need to have an experienced radiologist or experienced clinician, or both, to interpret the MRIs," Shoemaker explains. "And the images can't be viewed in isolation. They need to be put in the context of the clinical picture of the patient in front of you. So while the MRI may be somewhat able to predict MS, if the clinical history or the clinical exam is not really supportive of that, then it's kind of inappropriate to make a diagnosis."
Lesions are, however, a strong predictor of the disease. According to a 2014 report in Neurology, the risk for developing MS is generally 60 to 80 percent when lesions show up in an MRI. If none are found on the scan, then the risk lowers to 20 percent.
In addition to an MRI, additional procedures may also be required to help confirm a diagnosis, such as a spinal tap, also called a lumbar puncture, to test cerebrospinal fluid. When MS is present, the fluid often has a higher concentration of a certain type of immune proteins.
Shoemaker adds that in certain instances, more in-depth vision testing is needed.
"There's a procedure called an optical coherence tomography, which can sometimes demonstrate prior optic nerve injury, and similarly, there's a test called visual evoked potential, and that can also help dilate the optic nerve to see if there's prior injury as well, which may indicate MS."
Your doctor may also order blood tests if similar conditions to MS are also being considered.
Time and timing differentiate two types of MS
There are two main types of MS:
- Relapsing-remitting MS is exactly what it sounds like: New neurological symptoms develop caused by inflammatory attacks on myelin, called a relapse, followed by periods of recovery where the symptoms may improve, remain but not worsen, or go away. This period is called remission.
Relapsing-remitting MS is the most common form of the disease. According to the National Multiple Sclerosis Society, approximately 85 percent of people with MS are first diagnosed with relapsing-remitting MS. Most diagnosed with this type of MS are generally in their 20s and 30s.
- Primary-progressive MS occurs when there's no improvement in symptoms from the onset of disease. "There may be subtle improvements, but overall, the trajectory is continued worsening over a period of at least a year," Shoemaker explains.
This form of MS can be more difficult to diagnose since people with the primary-progressive type tend to have less brain scarring, more spinal cord scarring and less inflammation than those with relapsing-remitting MS. They also have more difficulty with mobility and everyday activities, and onset usually occurs in the 40s or 50s.
Whereas 80 to 85 percent of cases of MS are relapsing, primary progressive MS is about 15 percent of the cases at diagnosis, and a 50-50 split between men and women.
Know the risk factors
MS affects more than 2.3 million people globally. Though MS is not contagious or even directly inherited, some factors may increase the risk for this disease, including the following:
- Age. Most people diagnosed with MS, are between the ages of 20 and 50 years old, although MS can develop at any age.
- Ethnic background. Those of Northern European descent are at the greatest risk of developing MS, while Native Americans and those from African or Asian descent have the lowest risk.
- Gender. Although both men and women are affected by MS, women are at increased risk. In fact, according to the National Multiple Sclerosis Society, four times as many women have relapsing MS as men. "It tends to be a disease of women of reproductive age, so those from ages 18 to 50 receive the bulk of new diagnoses, with a median age of diagnosis being around 30 to 32," Shoemaker says.
- Genetics. Although MS is not inherited, the genetic risk for the disease may be, reports the National Multiple Sclerosis Society. The risk of developing MS is about 1 in 750 to 1,000 people in the general population. It increases, however, when a first-degree relative, such as parents, siblings and children, have the disease. And the risk is greater, nearly one in four, for identical twins.
- Geography. Areas farther away from the equator have more cases of MS. With less sun exposure, research indicates that people tend to have lower levels of vitamin D, which supports the immune function and protects against diseases like MS.
Shoemaker also cites other specific factors, either alone or in combination that may contribute to the disease, which include the following:
- Certain gene variations
- Exposure to the Epstein-Barr virus
- Low vitamin D or sun exposure
- Obesity during adolescence
Earlier diagnosis means better outcomes
Knowing what signs and symptoms to look for early has tremendous benefits.
"From some of the longer duration studies, detecting MS earlier and starting MS therapies earlier tend to improve the chances of having a good long-term outcome. Patients started on MS therapies earlier in their disease tend to have a lower likelihood of reaching certain disability milestones, like needing a cane or walker," Shoemaker says.
Although receiving an official MS diagnosis can be overwhelming, Shoemaker ensures that his patients understand how treatment can help. With nearly 15 Food and Drug Administration-approved therapies available, and new ones constantly being developed that are increasingly effective, management of MS continues to improve.
"We are at a point where we're happy with how good we are at controlling the inflammatory aspect of the disease," Shoemaker says. "Now we're working on trying to improve patients' overall quality of life so they can lead healthy, productive lives — as if they don't even have MS."