In the not-so-distant past, doctors treated strokes in an after-the-fact way. A stroke did its damage, and then — if the patient survived — a rehabilitation team stepped in to address the stroke's effects.
But in 1996, the Food and Drug Administration approved tissue plasminogen activator, or t-PA, which can dissolve blood clots that lead to ischemic strokes — strokes caused by an interruption in blood flow to the brain. The t-PA restores normal blood flow if administered promptly.
The timing of treatment is important, because lost time can lead to lost brain function.
Today, stroke specialists at Rush and elsewhere follow a timed, standardized set of procedures that require diagnostic tests and treatment to be given as quickly as possible.
This approach to stroke care has had a big impact on patient outcomes, both in terms of survival and quality of life. James Conners, MD, MS, a stroke neurologist at Rush, sheds some light on stroke survival and recent advances.
Stroke survival rate
Stroke survival rates can vary based on available medical care, which can depend on where a person lives.
“If a patient does make it to the hospital or gets to a comprehensive stroke center like Rush, then their odds of survival go way up, because we're able to get them treated accordingly,” Conners says.
The World Stroke Organization estimates that more than half of the 12 million people who suffer their first stroke this year will die as a result.
But that doesn’t necessarily reflect the survival chances for every patient or their long-term survival odds. Age, overall health and whether a person has had a previous stroke can all affect whether they survive. Survival rates also vary based on the type of stroke and which parts of the brain it affects.
For example, ischemic stroke, the most common type of stroke, has a much higher survival rate than intracerebral hemorrhage, a less common but more severe type.
Treatments and awareness have improved over time, and as a result, we started to see a decline in the number of total strokes each year, as well as stroke deaths. But the decline in stroke deaths has stalled in recent years — and even increased in some groups.
For example, a study found that Black Americans have not seen the same improvement in stroke survival over time and are 20% more likely to die within five years after having ischemic stroke than white Americans.
A different approach to stroke treatment
The improvement in stroke survival rates for several groups is due to many factors, including advances in treatment soon after stroke and stroke prevention.
"We now have multiple treatment options for patients who suffer from an acute stroke the first time, including clot busting medications like t-PA and endovascular devices that can reopen blocked blood vessels," Conners says. "We're also more aware of stroke risk factors, and we're better at controlling those with lifestyle modifications and, when necessary, medications.”
Better detection and treatment of high blood pressure have played significant roles, as well as new antiplatelet medications, statins to help lower cholesterol and improved control of diabetes.
Abnormal heart rhythms, like atrial fibrillation, or AFib, can also lead to stroke. New medications, such as blood thinners, may help patients who have AFib and are at risk of having blood clots form in the heart, which can dislodge and travel up into the brain, causing stroke. Blood thinners help prevent blood clots from forming.
Data has also shown that repair of a patent foramen ovale, a common heart defect, can reduce the risk of recurrent stroke in certain younger patients with no other stroke risk factors. PFO closure is yet another tool that we now have to prevent future strokes.
Technological advances = better survival rates
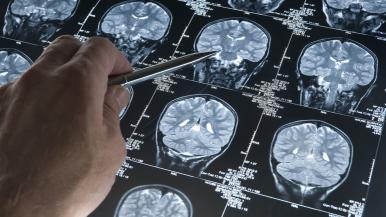
Today's imaging technology allows us to detect stroke within minutes of the first symptoms, see blood vessels in the brain that may be blocked and find out where blood is and isn't flowing.
"It’s helpful to know where blood flow is blocked when you’re considering an intervention to reopen the vessel, and it’s also helpful for us to understand the stroke mechanism, or what's causing the stroke," Conners says. "This all assists in the decision-making process and helps us improve outcomes."
To treat stroke successfully and limit damage to the brain and body, treatment with clot busting medications must begin within just a few hours of a stroke's onset.
Unfortunately, access to stroke neurologists is greatly limited at some hospitals, so many stroke patients don’t get specialized stroke care in a timely manner. That was one reason Rush created a telemedicine program, a partnership with community hospitals that brings world-class care to more patients.
"Telemedicine involves advanced videoconferencing and imaging technology to allow a stroke neurologist to assess patients remotely," Conners says. "The videoconferencing capability gives the added benefit of seeing and talking to the patient face-to-face. We can examine the patient and review radiologic imaging, which aids in a fast and accurate diagnosis. We are then able to quickly recommend plans of care."
If you suspect a stroke, don't delay: Each minute a stroke goes untreated increases the potential for disability and death. “Time is brain.”
How to survive a stroke
One of the most important ways to improve your chances of surviving a stroke is to be able to recognize the signs and symptoms.
The acronym BE FAST is an easy way to remember signs of stroke and what to do if you think a stroke has occurred. Here's what the letters stand for, according to the American Stroke Association:
- Balance: Sudden loss of balance is a common stroke symptom. Someone might seem unsteady or have an uneven walk.
- Eye changes: A person might have trouble seeing out of one or both eyes. It could be due to blurred or double vision or even complete vision loss.
- Face and head: The person may have numbness or weakness in their face. All or parts of their face may be drooping, or they may not be able to smile. They may also feel dizzy, have vision trouble in one or both eyes or have a severe headache with no known cause.
- Arms and legs: They have numbness or weakness in the arms or legs, especially on one side of the body. They may have trouble walking or lose coordination.
- Speech: The person may have difficulty speaking or understanding speech and feel confused.
- Time: If you see any of the signs above, call 911 or get to an emergency room or stroke center immediately for treatment.
The key take-home is that if you suspect a stroke, don't delay: Time is brain. Each minute a stroke goes untreated, 1.9 million brain cells die, increasing the potential for disability and death.
But with our current treatments we can prevent further damage and improve outcomes in many patients. Getting to a stroke center quickly for treatment could save your life or the life of someone you care about.
Take steps to reduce your stroke risk
To prevent a stroke, a healthy diet and moderate exercise are absolute musts. According to the American Stroke Association, a healthy level of physical activity for adults ages 18 to 65 should be at least 30 minutes of moderate exercise five days a week.
You can also use the following strategies to change the way you prepare your meals to help reduce your risk for stroke:
- Keep portions moderate.
- Drink more water; hydration is important for overall health.
- Limit your use of salt: Use vinegar, lemon juice, red pepper flakes, garlic and onions instead of salt.
- Limit use of sugar.
- Use canola, olive, corn or safflower oil in cooking.
- Buy fresh, lean cuts of meat, and trim the fat before cooking.
- Eat plenty of fruits and vegetables
If you’ve had a stroke before, you can also take steps to reduce your risk of having another stroke.
“Controlling blood pressure is important,” Conners says. “It’s the number one risk factor for stroke. Getting diabetes or high cholesterol under control, not smoking or quitting smoking, and a healthy diet and exercise are all major. These things can prevent a secondary stroke.”
FAQs about stroke
- Q: Can you die from a stroke?
- A: Yes, a stroke can be fatal, and many people die of stroke each year. It is currently the fifth-leading cause of death in the United States. But knowing the symptoms and seeking treatment quickly can improve your chances of survival.
- Q: What are the odds of surviving a stroke?
- A: The odds of surviving a stroke vary based on the type of stroke, the part of the brain that is affected and the individual patient. Recent data from the World Stroke Organization puts the survival rate for all strokes globally at about 46.6%, but that rate may be different for people in the U.S.
Delays in care can also decrease the odds of surviving a stroke, so seeking medical attention as soon as possible is crucial.
Following are more data points about stroke survival odds:- The odds of surviving an ischemic stroke are a bit higher with a survival rate — almost 57% in 2019. But the odds of surviving an intracerebral hemorrhage are significantly lower — only 15.34% survived that same year. Other types of stroke have different survival rates.
- The American Heart Association reports that the stroke death rate in the U.S. increased by 8.4% from 2011 to 2021. The actual number of stroke deaths also increased by 26.3% in those 10 years.
- But from 2021 to 2022, the stroke death rate slightly decreased based on data from the U.S. Centers for Disease Control and Prevention.
- There is some encouraging news from the University of Cincinnati. For patients with acute ischemic stroke, the survival rate five years after stroke improved from 47% in 1993-94 to 51.7% in 2015.
- Stroke has historically been the third-leading cause of death in the United States. But in 2020, stroke dropped to the fourth-leading cause of death behind heart disease, cancer and COVID-19. The CDC suggests that stroke was the fourth-leading cause of death in 2023 behind heart disease, cancer and unintentional injuries.
- Age, overall health, previous strokes and available medical care can all affect the odds of surviving a stroke.
- A: The odds of surviving a stroke vary based on the type of stroke, the part of the brain that is affected and the individual patient. Recent data from the World Stroke Organization puts the survival rate for all strokes globally at about 46.6%, but that rate may be different for people in the U.S.
- Q: How many strokes can a person have and survive?
- A: There is no set number of strokes a person can have and survive. It will vary from patient to patient. Even if a patient does not die, disability can start to build with each stroke, which worsens quality of life and odds of surviving another stroke.
Some people may have small strokes and not even realize it. "In those instances, oftentimes we'll see that accumulation of damage occurs,” Conners says. “We can even see something called vascular cognitive impairment where patients have what looks like any other type of dementia."
But Conners also notes that if a patient survives a stroke, they can often improve their condition with treatment, medication, rehabilitation and lifestyle changes. Some patients even make full or nearly full recoveries and can continue life as they did before they had a stroke.
- A: There is no set number of strokes a person can have and survive. It will vary from patient to patient. Even if a patient does not die, disability can start to build with each stroke, which worsens quality of life and odds of surviving another stroke.
- Q: What is the average life expectancy after surviving a stroke?
- A: According to a study published by the American Heart Association, the life expectancy of a patient who survived a stroke was reduced by 5.5 years on average. But this study was not conducted in the U.S. and does not reflect data collected after 2017.
Life expectancy after a stroke varies based on many factors. There are many treatments available today and lifestyle changes that stroke patients can make to improve their life expectancy and reduce their risk of further strokes.
“When we put someone on the right medication and address all their risk factors, we greatly reduce their risk almost close to the point of someone who hasn't had a stroke before,” Conners says.
- A: According to a study published by the American Heart Association, the life expectancy of a patient who survived a stroke was reduced by 5.5 years on average. But this study was not conducted in the U.S. and does not reflect data collected after 2017.
- Q: Can someone live a normal life after surviving a stroke?
- A: Yes, a person can live a normal life after having a stroke. "Some of this has to do with the size and location of the stroke and how much brain tissue we’re able to salvage early on,” Conners says.
If you’ve had a stroke, your physician can tell you more about what you can expect.
“It's always our goal to get patients back to what they were doing before the stroke,” Conners says. "Physical therapy, occupational therapy, speech therapy, working with our rehab physician colleagues — our goal is to try to get a patient to having no disability."
- A: Yes, a person can live a normal life after having a stroke. "Some of this has to do with the size and location of the stroke and how much brain tissue we’re able to salvage early on,” Conners says.
If you’d like to learn more about the care Rush provides for patients who have stroke or need follow-up care such as rehabilitation and help with lifestyle changes, visit our Stroke Care page.