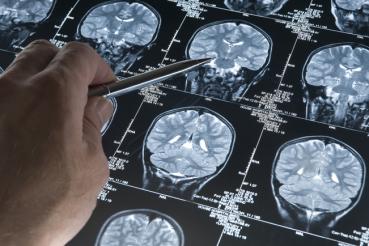
Like many people, David Bennett, MD, is concerned about Alzheimer’s disease, which currently afflicts an estimated 5.7 million people in the United States and is projected to develop in 14 million people in the U.S. by 2050.
Unlike most people, Bennett someday may be able to stop it.
The director of the Rush Alzheimer’s Disease Center (RADC) at Rush University Medical Center, Bennett is one of the world’s foremost Alzheimer’s disease researchers. In recognition of his accomplishments, he’s been chosen to receive the highest honor in the world for dementia research, the Potamkin Prize for Research in Pick’s, Alzheimer’s and Related Diseases, by the American Academy of Neurology and the American Brain Foundation.
He received the award April 22 at the AAN’s annual conference in Los Angeles. It’s a sign of his stature that when Bennett told the organizer of a conference in China he would have to cancel a planned talk there to receive the award instead, she rescheduled the conference around his availability.
Bennett – who also is the Robert C. Borwell Professor of Neurological Science at Rush Medical College – has been pursuing a solution to Alzheimer’s disease, the leading cause of dementia, since the early 1990s. He currently is the primary investigator of eight different studies funded by the National Institutes of Health, and a co-investigator on more than a dozen others. (He also serves on several National Institutes of Aging committees, including the National Advisory Council on Aging.)
He’s building on his quarter century of research discoveries to identify specific proteins in the body that affect the development of Alzheimer’s disease, so that he and other researchers can design treatments that target those proteins and prevent Alzheimer’s from occurring.
He doesn’t just want to cure Alzheimer’s – he wants to prevent it
“It’s a terrible disease,” says Bennett, who has been caring for Alzheimer’s patients and their families for more than 30 years. “Of all the things that happen to older persons, the number one thing the vast majority wants to prevent is the loss of cognition. They don’t want to lose their ability to plan for the future and their ability to remember the past, the things they’ve done and the people they love.”
The human brain has an extraordinary ability to rearrange neural connections as it learns and adapts to disease and injury. By the time Alzheimer’s dementia overwhelms that ability and begins robbing people of their thoughts and memories, the damage it has caused is so great that it has thwarted massive efforts to find a cure.
“Between 1993 and 2002, five drugs were (FDA) approved for the symptomatic treatment of Alzheimer’s disease, and they don’t work very well,” Bennett says. No drug treatments for Alzheimer’s have been approved since then.
“As a public health strategy, we have to prevent the disease,” he says. “However, people have it and will continue to get it, so we also need to develop better treatments.”
For more than two decades, he’s led unique ongoing major Alzheimer’s studies
Bennett started and leads two ongoing studies funded by the National Institutes of Health — the Religious Orders Study, which examines memory loss in Catholic nuns, priests and brothers from across the United States; and the Rush Memory and Aging Project, which is a similar study of lay persons in northeastern Illinois. Since they began testing participants in 1994 and 1997 respectively, the two studies between them have enrolled more than 3,500 older people to date and continue to recruit participants.
“I just signed two consents this morning,” Bennett says as he sits in his corner office on the tenth floor of a building on the Rush campus, facing windows that look out at streaks of the setting sun trying to break through April rain clouds.
Participants do not have dementia when they enroll in the studies, but some develop it over time. The studies annually collect clinical information (including brain imaging) and biospecimens (blood, etc.) from the participants. The annual detailed data collection for nearly a quarter century makes these studies unique.
Even more noteworthy is that all participants agree when they enroll in either study to donate their brains to the research after their deaths. Participants who are autopsied at Rush also donate spinal cords, nerves and muscle.
“These are the only two studies in the world of risk factor for Alzheimer’s disease in which all participants are brain donors,” Bennett says. To date, more than 1,500 deceased participants have donated their brains.
By comparing the pathology (anatomical damage) in the brain samples of people who did and didn’t develop Alzheimer’s disease with the clinical data recorded during their lives, and examining what causes these changes, Bennett and other researchers have made a trove of new discoveries about how and why Alzheimer’s develops and progresses and why some people develop the disease's brain pathology but do not exhibit memory loss. Further, by generating numerous layers of molecular data, the studies are yielding insights into novel ways to treat and prevent not only Alzheimer’s disease but many other common brain diseases.
‘I don’t think I could have done this anyplace else’
To make this work possible, the RADC’s staff of about 150 includes not only neurologists like Bennett, but geriatricians, neuropathologists, computational neuroscientists, geneticists, statisticians, neuropsychologists, epidemiologists, physicist and biomedical engineers. They work closely with a community engagement team, managers, coordinators, field and laboratory technicians, information systems analysts, and administrators.
In addition to drawing on the two studies for its own research, the RADC shares the data and biospecimens from these studies with researchers around the world to advance the development of therapies to treat and prevent memory loss and dementia. “The resources that we generate here are extraordinary and unique. They don’t exist anywhere else in the world,” Bennett says.
“The one thing you have to have for what I do is patience,” continues Bennett, who was only 33 years old when the National Institute on Aging funded the Rush Alzheimer’s Disease Center in 1991. “I don’t think I could have done this anyplace else. Rush’s support has allowed us to take these long view arcs that are almost impossible to achieve at other institutions.”
A massive study in Brazil seeks to better understand Alzheimer’s in minorities
The risks for Alzheimer’s disease, and most likely the solutions for it as well, differ greatly among ethnic groups, and researchers need to understand those differences. However, many black individuals and Latinos are reticent to donate their brains for study after their deaths due to cultural sensitivities.
Of the 1,500 donated brains at Rush, only about 40 are from black study participants and another 40 are from Latinos. There are another 35 from three other cohort studies conducted by the RADC.
“It will take many more years to achieve sufficient numbers to conduct the kind of work in minorities being done with the donations from whites,” Bennett says.
To address this problem, Bennett is looking to Brazil, which requires that anyone who dies in the country without a cause of death undergo an autopsy. He’s partnered with colleagues at the University of São Paulo – named for and located in the teeming city of more than 12 million in southeast Brazil – which conducts autopsies on more than 13,000 people a year.
With an $11.2 million grant from the NIH, a team of researchers at Rush and in São Paulo, along with colleagues at Columbia University and the Harvard School of Public Health, will collect 10,000 brains. Using advanced genetic analysis techniques, they’ll characterize each brain by its mix of African, European and Native Brazilian ancestry (Latino ethnicity represents various combinations of these three ancestries), and identify how genetic variants of each ancestry are associated with the brain pathologies of the most common neurodegenerative conditions of aging, including Alzheimer’s, stroke, and Parkinson’s disease.
This approach will cover the full range of each condition, from people without symptoms to those with mild or severe cognitive impairment prior to death. Identifying genetic variations that cause brain pathology and symptom development will greatly increase understanding of how these conditions affect blacks and Latinos, both in Brazil and the U.S.
For example, among non-Latino whites in the U.S., the inclusion of a gene known as ApoE4 in a person’s genome (genetic composition) is the greatest risk factor for developing Alzheimer’s disease. “If you are African American, you are almost twice as likely to have the E4 genotype, but the risk associated with it is much smaller,” Bennett says.
“The opportunity is Brazil is extraordinary,” Bennett says. “There is no other place in the world where a study of this size could be accomplished. It will markedly speed up the pace at which we can build a drug discovery pipeline with the potential to identify different genomic causes of disease in African Americans and Latinos and potentially therapeutics for them.”
He’s helped identify the main risk factors for Alzheimer’s disease
The first wave of published research papers that Bennett and his colleagues at the RADC produced, from 1994 to 2008, focused on risk factors for Alzheimer’s disease and the neurobiology of the illness. “This thing we call clinical Alzheimer’s dementia is an extraordinarily complex set of different factors going on in your brain,” Bennett says.
“Some factors are driving you to lose memory, and other factors are helping protect you. They include experiential, psychological and medical risk factors, in addition to multiple neuropathologies and resilience factors in the brain.”
Bennett’s group was the first to identify many of the factors that increase or reduce the risk of Alzheimer’s disease dementia. Just a few of the many discoveries they have published include that more cognitive activity is associated with a reduced risk of Alzheimer’s dementia; that more purpose in life was is associated with a reduced risk; that psychological risk factors, such as neuroticism, depressive symptoms and loneliness, are associated with an elevated risk; and that diabetes likewise is a risk factor.
Physical damage of Alzheimer’s often doesn’t cause memory loss
Alzheimer’s disease produces pathology — physical damage — in the brain, such as blood vessel disease or the buildup of harmful proteins known as amyloid plaques and neurofibrillary tangles. Because everyone in the two long-term Rush studies is an organ donor, the RADC has an unprecedented opportunity to examine how the wide range of risk factors is related to brain pathology.
The RADC team was the first to report that mixed pathologies are the most common cause of Alzheimer’s dementia in older persons. On the other hand, one of the biggest discoveries that Bennett and his colleagues have made is that brain pathology doesn’t mainly determine whether or not a person becomes demented, and how far dementia progresses.
They were the first to report that persons without any cognitive impairment whatsoever often develop brain pathologies. This work contributed to the evolution of new criteria for Alzheimer’s disease adopted by the field in 2011 and again in 2018.
“You can get a brain full of pathologies without losing much cognition, or you can have very little pathology and lots of lost cognition,” Bennett says. “We’ve found numerous risk factors of cognitive decline and dementia that aren’t related to any brain pathology. Those risk factors are doing something, but it’s not causing any pathology that we know of today.”
These findings date back to 2003, when Bennett and his colleagues published the first research paper that combined risk factors with pathology and cognitive decline in the same model. In this paper, the risk factor was the aforementioned ApoE4 gene, which does clearly cause the development of Alzheimer’s pathology.
In subsequent papers that they’ve continued to publish to this day, however, the researchers have reported that while they could correlate a risk factor with cognitive decline and the development of dementia, they couldn’t match the decline with brain pathology. “That means that there are systems in the brain that determine whether or not you lose cognition completely separate from the development of known brain pathologies,” Bennett says.
“There probably aren’t a lot of them, and the question is, ‘where you find them?”
His research now focuses on what causes resilience in response to Alzheimer’s
Resilience is the term Bennett and his colleagues use to refer to cognitive change that cannot be explained by common brain pathologies such as plaques and neurofibrillary tangles. A person may be more or less resilient, resulting in slower or faster loss of cognition.
Bennett wants to know why some people are more resilient, others are less, and how to increase resilience in everyone. He thinks that resilience could be an approach to therapy that could prevent loss of cognition from all common brain diseases.
“Resilience doesn’t care what brain pathology or injury is developing,” Bennett says. “All people have some resilience. It’s just that some have more and others less. If you can augment it, you can actually counter the effects of multiple different brain diseases,” including Parkinson’s disease and stroke, in addition to Alzheimer’s disease.
Therefore, Bennett and his colleagues are focusing their work on identifying targets – factors that affect resilience – and trying to determine if they’re “drug-able,” that is, if they can be affected by a medication that eventually could be used in human beings. In fact, it’s been his long-term goal since the late 1990s.
He’s found two proteins that affect resilience, and he’s looking for others
Bennett expects most of these therapeutic targets to be proteins in the brain that will be found to be associated with “a faster or slower rate of memory loss, a higher or a lower risk of Alzheimer's disease. Then we’ll try and move them in the direction of a healthier level of the protein and hope that it will improve people’s cognition.”
He already has identified two such proteins, known as Ak4 and ITPK1, which are associated with memory loss despite not being related to any brain pathology. The association is with higher levels of Ak4 and lower levels of ITPK1, so blocking the former and raising levels of the latter may increase resilience and help maintain cognition.
“There are first two and the strongest ones we have found to date. There’ll be a lot more,” Bennett says.
Developing ‘cognition in a dish’…
“The reason we’re interest in proteins is that proteins are the most common target for therapeutics,” Bennett explains. “We’ve identified targets for resilience, but to see if it’s drug-able, I need to put it in some kind of high throughput model.
“I basically need cognition in a dish.”
Therefore, Bennett’s team is taking tissues donated by participants in the two long-term Rush studies, extracting cells and reverse engineering them back to being pluripotent stem cells, which can develop into any kind of cell in the body. Then they’re stimulating these cells to become different types of brain cells that can be studied in a laboratory dish.
He’s developing these cells from tissue taken from deceased participants whose medical history he knows well, including knowing how resilient they were when they were alive. “The question is, can we develop a method of challenging those cells and measure something that correlates with the known resilience?” Bennett asks.
In other words, he and his team want to find a way to mimic resilience in the cells growing in the dish. Since the cells came from the deceased participants, they can match what is found in the dish with what is known about the participant.
“When we have a proxy for resilience in a dish, then we can take the cells and manipulate genes that affect the production of Ak4 and ITPK1 and other proteins to see if we affect resilience in the desired direction,” Bennett says.
“What we’re talking about now was science fiction when we started. It’s science fiction even to a lot of my colleagues today.”
…may lead to therapies that can protect the brain from becoming demented
If he can make what once was science fiction a reality, Bennett then could move on to similar experiments in flies and mice that would be precursors to possible clinical trials of the intervention in human patients. In theory, the interventions would alter the levels of multiple proteins identified as Alzheimer’s risk factors, up or down as needed to increase resilience.
The therapy wouldn’t be limited to people with levels of those proteins that put them at Alzheimer’s risk. “The interventions are for everyone,” Bennett says, because even people with protective levels of a given protein might benefit from more protection.
“This has been the culmination of over two decades worth of work,” he says. “What excites me is that for a long time it wasn’t really clear how we were going to get to that therapeutic pipeline, but over the last five years it has become very clear in my mind. The technology has been developed, we have the resources here at the Alzheimer's center, and we are finally moving into the realm where we can actually see the light at the end of this tunnel.
“I’m not saying we’re going to get there any time soon, but at least the roadmap that we need to follow has become very, very clear. It’s very exciting, and I hope I’m around long enough to see those drugs come out and be helping people.”