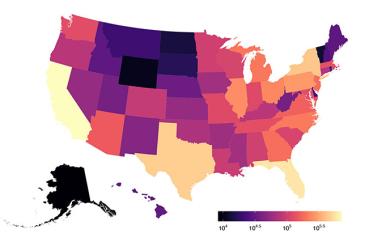
According to some estimates, Black adults in the United States have more than double the risk of developing Alzheimer’s disease than their white counterparts. What accounts for the gap?
Lisa Barnes, PhD, a cognitive neuropsychologist in the Rush Alzheimer’s Disease Center and the Alla V. and Solomon Jesmer Professor of Gerontology and Geriatric Medicine at Rush Medical College, is working to understand it — and working toward achieving equity in how we examine brain health.
Barnes is the principal investigator on a long-term brain health study of more than 800 Black Chicagoans age 65 and older. Her article about diagnosing Alzheimer’s, “Alzheimer disease in African American individuals: increased incidence or not enough data?” was published in the journal Nature Reviews Neurology in December.
The trouble with cognitive testing
Barnes says that studies of aging and brain health enroll thousands of participants, but relatively few of the studies focus on Black older adults.
“That means that data obtained from white populations is treated as the gold standard for diagnosis and research — but there’s a real issue with using that data to define what is ‘normal,’” she explains. Additionally, the small amount of data on Black older adults makes it difficult to determine whether Black populations are truly more at risk than white populations.
Diagnosing Alzheimer’s dementia is a complex process that involves testing for memory and thinking problems; determining whether those problems interfere with everyday activities; and gathering information from a neurological exam, lab tests and brain imaging to help rule out other causes of cognitive impairment.
There are particular equity issues with cognitive testing, however. “Often, the diagnostic process will fail to take into account documented disparities in how diverse participants perform on cognitive tests,” Barnes says.
The tests can be culturally biased in terms of content or the way they’re conducted. For example, “if an older Black patient grew up in the Jim Crow South and as a result had lower-quality education, tests that were created using a differently educated white population may result in an impaired score for the Black patient — when their score is actually within normal range, considering the cultural context,” Barnes says.
Another disparity related to cognitive testing is that people’s brain health can be affected by factors like childhood trauma. Black people who report having experienced racism have increased rates of conditions like depression, type 2 diabetes and high blood pressure, all of which can affect cognition.
“Studies of Holocaust survivors have shown that early-life traumas leave a mark and can impact brain and cognitive health,” Barnes says, “so we know that people’s life histories matter.”
Environmental factors can also have an impact on brain health. For example, we know that physical activity and a healthy diet can help protect against Alzheimer’s — but both can be difficult to achieve for people who live in disinvested neighborhoods that lack grocery stores and safe places to exercise. Barnes and her team are investigating how to measure the impact of those factors on cognitive performance.
Longitudinal studies (in which participants take tests at regular intervals across a period of time) conducted by the Rush Alzheimer’s Disease Center show white participants performing at a higher level on cognitive tests than Black participants — but they don’t show a difference in how each population’s performance changes over time.
“If Black older adults are at greater risk of Alzheimer’s dementia, shouldn’t they decline at a faster rate over time?” Barnes asks. “We’re not seeing that in our studies. So we need more data in order to clarify the finding.
“What we really need to know is whether people have actual markers of disease in their brains as they age, but we just don’t have enough Black people who have agreed to donate their brains after death so that we can measure these markers.”
Building trust to build understanding of Alzheimer’s
Barnes hopes to remedy the overall lack of data on Black populations with her study, now in its 17th year. In 2004, with National Institutes of Health funding, she and her team recruited 350 Black Chicagoans age 65 and older who had no diagnosis of dementia and agreed to complete cognitive testing and bloodwork every year.
“Trust is a big issue” in this community, she says, so during the study’s first five years she visited every participant in person to thank them and answer their questions.
It was a time-intensive approach, but it has paid off: “People feel invested in this work, and they know me — I’m like their granddaughter,” she says with a laugh.
“The relationship has gone a long way toward helping us retain people in the study over time,” which is crucial to tracking the same group of participants’ cognitive health for many years.
The trust Barnes has built with the participants in her study has enabled her to begin asking them about donating their brains for study after death. “We’ve had to educate people and their family members about donation, why it’s important and what we’re looking for.
“I tell them that this is how we’re going to discover a cure for this disease.” About half of the study’s current participants have agreed to donate their brains at the time of death.
To increase participants’ comfort with the study process, Barnes’ team visits them in their homes to conduct all cognitive tests and blood draws. “That removes a large barrier,” she says.
“Many people don’t have access to reliable transportation, or don’t want to navigate a complicated medical center. We do testing in people’s homes and bring the data back to Rush.”
Barnes and her team are also working to inform the community about their research. They regularly make presentations for churches, senior buildings, civic groups and other spaces where Black Chicagoans gather.
“We start with the basics: What is research, why do we do it, and why is it important for you to be included? We talk about Alzheimer’s and how it’s affecting older Black people at a higher rate. We talk about healthy aging. And we are very transparent about what we’re finding and how the community has contributed.
“People get to know us as faces of Rush, and know that we care about them. All those things together help strengthen trust and relationships.” The resulting word of mouth in the community has helped Barnes recruit new participants and more than double the size of the initial study cohort.
In pursuit of equity
Ultimately, Barnes says that her goal is equity in the discussion and study of aging and brain health. “Comparing all other racial or ethnic groups to whites isn’t equitable — and can make people in those other groups feel like they don’t want to participate in research at all.
“My dream is that we can center diversity, or decenter whiteness, so that everyone is on the same playing field. We do that by increasing the number and diversity of people involved in studies, raising awareness in the community about how this disease doesn’t discriminate, and identifying the things that might help to mitigate it.”