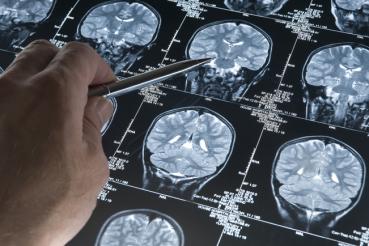
The outlook for people with Parkinson's disease is improving
Healthy Living
A Doctor Who's There for You, 24/7
New Rush Concierge Medicine physician Sam Panjwani, MD, emphasizes in-depth patient relationships