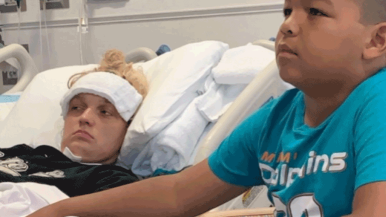
Ashleigh Hitterman speaks a little more slowly now. But she speaks clearly, and strongly, and she speaks for herself.
“I don’t think I’ve ever heard of anyone having to relearn how to talk,” Hitterman said. “That’s a weird process.”
There was a time when it wasn't clear the 30-year-old would ever speak again. Or walk. Or move at all, after a mysterious stroke in 2019 left her with locked-in syndrome, a rare condition causing paralysis of nearly all the voluntary muscles.
A terrifying mystery
Doctors in Indiana thought Hitterman had overdosed.
When her boyfriend found her unresponsive on July 4, 2019, at his home, he called paramedics, who took her to a local hospital. She was repeatedly treated with naloxone for a suspected opioid overdose.
“My boyfriend and my mom kept saying that I didn’t use drugs,” she said. “I’ve never used drugs, never once in my life.”
A CT scan showed the true cause: a blood clot in the basilar artery, a large blood vessel located in the back of the brain. She was airlifted to Rush University Medical Center for treatment.
Hitterman was lucky. Her Rush neurosurgeon, Stephan Munich, realized quickly she had locked-in syndrome. People with locked-in syndrome are unable to speak or move, appearing comatose, but are conscious and can think and reason. Unable to communicate with medical staff or loved ones about their status, some can be trapped for days or weeks before being correctly diagnosed.
“The only movements people who are locked in can make are vertical eye movements,” Munich said. “When she came in, we were asking her to lift an arm, to respond: nothing. Then I opened her eyelids, and said ‘Ashleigh, look up.’ She looked up right away. And I said, ‘Look down.’ And she looked down right away.”
A true 'Hail Mary'
The outlook for patients with locked-in syndrome is not encouraging: A 2003 study of 14 patients found that only 20% of patients regained some motor function and 28% regained some speech after rehabilitation. Most, however, must learn to communicate through eye movement or computer software and remain at least partially paralyzed.
By the time Hitterman was admitted to Rush, she had experienced symptoms for nine hours, limiting treatment options. Hitterman’s only option at that point was surgery to have the clot removed in the hopes of re-establishing blood flow to the affected part of the brain.
“It was sort of a Hail Mary,” he said. “When there is blood restriction to a part of the brain, that part dies at different rates based on whether there are other compensatory ways for that part of the brain to survive.”
That being said, nine hours out is a long time, but with a basilar artery occlusion we do it because it’s the only chance somebody has.”
Munich was able to remove the clot and fully re-establish blood flow within the artery. Due to the damage caused by the stroke, Hitterman’s brain began to swell. Two days later, she underwent surgery again to have a piece of her skull removed, so her brain could swell without causing further damage.
Hitterman’s team told her mother, Dee Panozzo, that her chances of full recovery were uncertain.
“I said, no, just no,” Panozzo said. “She has an 8-year-old son. She has to fight.”
A painstaking recovery
The first part of her body she was able to move was a fingertip.
Following her surgeries, treatment moved to supportive therapy. She received a tracheostomy that kept her breathing comfortably, and a gastrostomy tube in her abdomen to allow her to receive food.
She was transferred to the Shirley Ryan AbilityLab to begin rehabilitation but had to return to Rush five days later. Cerebrospinal fluid had begun collecting in her brain, and Munich put in a shunt to drain it.
Speech-language pathologist Itza Davila brought in a board with letters (called an eye gaze board) and taught her to blink to spell out what she was trying to say.
“It was so frustrating. I had to blink out, letter by letter, word by word, at the board,” Hitterman said. “It took forever.”
Panozzo stayed by her side every day at the hospital, and then at rehab, as a fierce advocate and caregiver.
“I had a rule that no one was allowed to say anything negative in front of her,” Panozzo said. “I would keep saying, ‘You know, she can hear you.’”
Slowly but surely, Hitterman began to make steady, yet extraordinary progress.
Moving forward
“I’m never going to be back to normal,” Hitterman said. “I hate that question, ‘When are you gonna be fully recovered?’ I don’t think that’s ever going to be a reality.”
By any medical measure, Hitterman’s recovery is astounding. She is walking, talking, driving, working, living independently and caring for her now 11-year-old son. But she still bears some markers of the stroke that nearly took her life.
“I get exhausted a lot, I think that’s the main thing. My balance is off,” she said. “But I stopped using a cane, unless I’m taking a long walk. Or drinking.”
Munich says that reestablishing blood flow to Hitterman’s brain after her stroke, and the aggressive treatment to treat her brain swelling were integral to her care — but it was Hitterman herself who did the heavy lifting.
“Pushing through rehab and all the efforts that she put into that,” he said. “I think because of our efforts she was given the best chance, but I think it was really her efforts that put her where she is now.”
He also credits Panozzo for her caregiving skills.
Panozzo "was at her bedside the entire time, making sure she was turned, making sure her incisions were cleaned,” he said. “Her never giving up, both of them never giving up, was key.”
Looking back, Hitterman says her recovery was as mental as it was physical.
“I’ve never been a positive person,” Hitterman said. “Actually, kind of the opposite. But I always thought about ‘when’ I was gonna start moving, ‘when’ I was gonna start talking. Not ‘if’, ‘when’. I’m not saying everybody can recover, but everybody shouldn’t lose hope.”