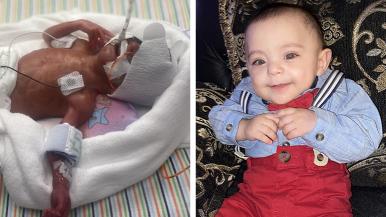
Gabriel Nino Gonzalez was born at 23 weeks — 17 weeks shy of the 40-week gestation period that is considered full-term and necessary for development. Seventy to 80% of babies born this early either do not survive or have long-term disabilities. Scary for his parents, Susana and Sergio Nino Gonzalez of Aurora — but “routine” to Rush Copley’s level 3 neonatal intensive care unit, or NICU.
“This is what we do,” says Rush neonatologist Naveed Khan, MD.
Level 3 for emergencies
Mother-to-be Susana was only slightly more than halfway through her pregnancy when it became clear that her baby would not wait to be born. Knowing the risks of having the baby that early, she cried. “I was so scared and sad,” she recalls.
But the level 3 NICU exists to handle such emergencies with highly skilled nurses and a neonatologist always present to help a newborn make the transition to life outside the womb.
In Gabriel’s case, all the appropriate team members and equipment were there at delivery, including nurses, a respiratory therapist and a neonatologist. Once delivered, the baby was stabilized and brought to the NICU.
Teams collaborate to meet needs
“Our obstetrics, maternal-fetal medicine and neonatal teams all collaborate,” Khan says. “Because of the team approach, the baby has everything he needs.”
Premature births are common in the NICU but Gabriel’s condition was extreme. Because he was born so early, his vital organ systems were not fully developed, and he was placed on a ventilator.
Although he was at the highest risk for potential complications, he did much better than expected. “His lack of additional severe complications is a testament to everyone involved in his care,” Khan says, noting the NICU nurses, respiratory therapists, dietitians, physical and speech therapists, social workers, care coordinators and pediatric specialists who were part of his care team.
“In addition to all this coordinated support, Gabriel had the blessing of having involved parents,” Khan says. “Their presence helped him in his hospital course and equipped them for his future needs.”
Gabriel’s mom provided breast milk, and both parents were involved with hands-on care, including “kangaroo care” — the skin-to-skin contact that offers both bonding and medical benefits to the baby, including stabilizing the baby’s heart rate and improving his breathing pattern.
Gabriel was a week old when Susana held him for the first time. “It was scary,” she says. “He was so tiny.” He weighed less than two pounds.
A substitute for the womb
As his lungs developed, Gabriel was weaned from the ventilator, and after 119 days in the NICU, he was discharged to home. Born weighing 1.5 pounds and just 12 inches long, he was discharged at approximately 40 weeks gestational, having grown to more than 6 pounds and 18.5 inches. Even though he needed oxygen for home at the time of discharge, he needed no additional medications and had no other significant complications. While Gabriel’s story is not unique, his outcome was extraordinary given the challenges he faced after leaving his mother’s womb so early.
The womb houses and nourishes the baby until he or she is ready to be born, providing hormones, the right temperature, nourishment and oxygen.
“The womb is a magical place for babies to develop,” Khan explains. “The womb can’t be replaced, but when babies are born prematurely, the NICU does its best to replicate womb-like conditions. Under the care of the NICU team, Gabriel did amazingly well. With exceptional nursing care, he was able to grow in an environment outside of the womb.”
“It was a bad experience but at the same time it was a good experience,” Susana says of the 17 weeks in the NICU. “It was hard to see my baby like that with all the wires, but they did what they had to do to help him.”
Strong baby, strong care
Like all preemies, Gabriel will be monitored as he grows to ensure he is meeting developmental milestones and receives appropriate resources to overcome any delays.
“Gabriel’s story shows how strong he is as a young baby and how strong we are in the care we provide,” Khan says. “We are proud and happy that he did so well.”
“I’m so glad to have my baby,” Susana says. “It was a long, long journey but he’s so strong. He went through a lot. We went through a lot. I cried a lot. The NICU was so helpful. They were so, so, so great with him and with me, explaining everything he needed. It was a rollercoaster, as they said it would be. He had good days and bad.
“Now, he smiles a lot when you talk to him and he loves to be held. He’s our little miracle.”