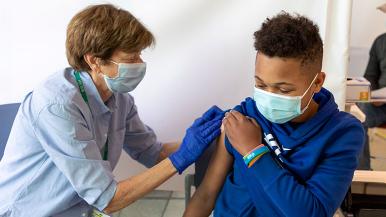
While parts of life in the United States have returned to normal, COVID-19 still is spreading in the country, especially in areas with low rates of vaccination against the disease. To provide an update on the state of the pandemic in the United States, John Segreti, MD — a hospital epidemiologist and the medical director of infection control and prevention at Rush University Medical Center — answered questions about the delta variant, breakthrough infections, vaccines for young children and more.
President Biden held a Fourth of July event at the White House celebrating both Independence Day and the United States’ progress against COVID-19, but he acknowledged that “COVID-19 has not been vanquished” and said “we’ve got a lot more work to do.” What’s your own assessment of the current situation?
Segreti: We’ve improved a lot, but we’re stalling in our fight against COVID, because people aren’t getting vaccinated. Some people don’t want to be vaccinated for a variety of reasons, many of them not accurate, and some people are not getting vaccinated because they’re waiting for more information, and some people are having trouble getting access to vaccinations.
That third group is getting smaller and smaller, but we need to make sure that everyone who wants to be vaccinated can get vaccinated easily and that we are doing everything we can to facilitate that. For the people waiting for more information, we need to get them the information they need so they’ll decide to get vaccinated. For people who do not want to get vaccinated, we need to educate them, but I’m not sure what more we can do.
The biggest concern about the pandemic right now seems to be the delta variant that first was identified in India. Why is it causing so much alarm?
It’s a concern because it seems to be more transmissible than other strains of the virus, and we just heard that it’s now the predominant variant here in the U.S., accounting for about 52 percent of all the COVID strains.
The good news is that we have evidence that the vaccines seem to work against it, especially in terms of preventing hospitalization and deaths. There’s some evidence from Israel that the vaccines may not be as effective in terms of preventing disease, but still very effective in terms of preventing hospitalization and death. Vaccination is the only way to avoid having this particular strain become more of a problem.
How common are breakthrough infections among fully vaccinated people, and how are delta and other variants affecting this risk?
The estimates are still that 99 percent of the people hospitalized with COVID are not vaccinated, and 99 percent of the people dying of COVID are not vaccinated. You’d expect a fair number of breakthrough infections given the total number of vaccinated. That’s not surprising at all, and it doesn’t mean the vaccines aren’t working, especially with regard to preventing hospitalizations and deaths. The percentage compared to the number of vaccinated people is very small.
What conditions or behaviors put people at risk of a breakthrough infection?
Any activity that’ll increase your risk of getting infection is the same, whether you’re vaccinated or not vaccinated. Being in a crowded area indoors is probably the riskiest situation, but the number of vaccinated people getting infected will be much, much less than the unvaccinated.
As far as conditions, the big one is if a person is immunosuppressed, especially transplant patients. If you’re on high-dose steroids, you’re getting cancer chemotherapy, you’re getting treated for leukemia or you have a bone marrow transplant, you have greater risk of getting infected, even with the vaccine. Your immune system may not work as well. You should still take the same precautions as people who aren’t vaccinated.
In part due to concerns about the delta variant, leaders of the World Health Organization recommended a few weeks ago that even vaccinated people continue to wear face masks to protect themselves, but then the director of the Centers for Disease Control and Prevention reiterated the CDC’s guidance that fully vaccinated people don’t need masks in most situations. What’s the reasoning behind these differing recommendations?
It's a different audience. The World Health Organization is talking to people all over the world, including developing countries where rates of vaccination are incredibly low, one or two percent of the population, as opposed to the U.S. and parts of western Europe where they have 60, 70, 80 percent of their population immunized. They issue recommendations to everybody, not specific countries. Here in the U.S., where more than two-thirds of adults have gotten at least one dose of the vaccine, we’re in much better shape.
What do you recommend as far as mask precautions for vaccinated people, and what do you recommend for unvaccinated people, including children too young to get the vaccine?
The CDC recommendations for easing masking were for fully vaccinated people, and kids under 12 can’t be fully vaccinated. On the plus side, children don’t get very sick with COVID, and hospitalization and death are unusual, although it’s not zero. I would still be very cautious with kids under 12 and anyone over 12 who isn’t vaccinated. If they’re inside in a crowded area, they still should be masking and taking distancing precautions.
When are vaccines likely to be available to the children under age 12?
It’s still expected we’ll see vaccines for kid under the age of 12 by the end of the year. Some people are saying we might get some information by the end of the summer, beginning of fall, but those are just guesses. It all depends on how well the studies of the vaccines in younger children go, if they’re able to enroll enough people and how many of them get sick.
The U.S. began vaccinating people more than seven months ago. What’s the current thinking about the vaccines’ longevity and the need for booster shots?
Lab studies suggest that the people who are vaccinated might have more durable protection than was originally estimated, because the cell-mediated immunity (the disease-fighting cells in the immune system) lasts longer than just immunoglobulin (antibodies), but decisions about whether or not boosters are needed will be made based on ongoing studies with the vaccinated cohort (participants in the vaccines’ clinical trials), who are being followed to see how many of them get sick. The latest update I saw was that the results still were very good after eight months
A few months ago, I would have been very surprised if we didn’t need boosters, but now I’m not so sure. The vaccines in the U.S. have held up a lot better than people predicted, so we still don’t know if the boosters will be needed. There are certain vaccines made outside the U. S. that don’t seem to work as well, and boosters may be needed in other countries.
The last time we talked, you said the vaccine from Novavax might be a good candidate for booster shots. In mid-June, Novavax announced strong results for the clinical trial of the company’s vaccine. What impact do you think this vaccine may have at this point?
It’s a much, much more traditional method of making vaccine. It doesn’t use the mRNA technology (that the Pfizer and Moderna vaccines use), so hopefully it will convince people who were concerned about mRNA technology to take the new vaccine. Because it doesn’t have nanoparticles like the mRNA vaccines, it doesn’t have to be frozen at -20 or -80 degrees Celsius, and it’s much more stable. It can come in preloaded syringes, so doctors can give it in their office instead of people needing to make a trek to get vaccinated. Hopefully, they trust their doctor and their doctor can convince them to get vaccinated while they’re in the office for something else.
The Biden administration recently announced a $3.2 billion program to speed up development of antiviral drugs to treat the disease. What’s your assessment of the potential of these drugs — can they make a significant difference?
The biggest failing in the response to COVID-19 so far has been the lack of an effective antiviral drug that’ll change the course of the illness. The therapeutic end has lagged behind the vaccines. If you can start taking a medication by mouth that’s safe and decreases the risk of you going to the hospital, that’ll be huge, and if you’re in the hospital and that medication will improve the chances of your survival, that’s huge.
Pfizer has started studies, Merck has a candidate they’ve started studying, but those take time. People are looking at lots of different drug candidates, and maybe one of them will emerge as something that’ll get approved, but it’s still a long ways off.
It’s now been more than a year and a half since China first reported cases of what we now call COVID-19. Do you think that someday it will stop being a serious health threat, nationally and globally, and how do you think we’ll reach that point if we do?
Yes I do, and I think it’ll probably be sooner than later. I think that probably in six to 12 months, most countries will be living with this virus. More people will get vaccinated, more people will have been infected and have natural immunity, and unless we get a strain that’s a lot different than the others and causes more illnesses, I think it’ll be part of the background of respiratory viruses that we have had in the past.