Learn more about spinal fusion surgery
In the most literal sense, spinal fusion is exactly what it sounds like: an operation in which two or more vertebrae are permanently joined together.
But according to Frank M. Phillips, MD, an orthopedic spine surgeon at Rush University Medical Center who has been a leader in research to improve the tools and techniques used for the procedure, there's more you should know about fusion surgery.
1. Fusion can often be done minimally invasively.
Compared to just a decade ago, fusions today involve far less trauma to patients.
A traditional open fusion involves a large incision in the back to expose the spine, then cutting through and retracting the thick spinal muscles.
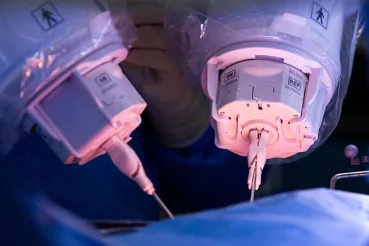
For minimally invasive fusions, the surgeon requires only a small incision (1 to 2 inches) and maneuvers special instruments between the muscles, pushing them aside and protecting them, to reach the spine.
Spinal implants are then placed with specialized techniques through this small incision. Microscopes enable the physician to view the area with magnification, allowing for more surgical precision.
Studies have shown that after minimally invasive fusion, patients experience less blood loss, less postoperative pain, lower risk of infection, shorter hospital stays and a faster recovery; many are able to leave the hospital the day after the procedure, compared to up to a week of hospitalization for traditional surgery.
Phillips was involved in the development of several minimally invasive procedures that are increasingly used today for spinal fusion, including a lateral approach that involves accessing the spine through an incision in the side of the body to avoid any disruption of the back muscles.
2. Many patients return to normal activities.
Phillips says many patients express concerns about having spinal fusion because they think it will keep them from participating in the activities they enjoy.
In fact, for fusions involving only one or two levels (each vertebra represents a level of the spine), which comprise roughly 80 percent of all fusions performed, most patients are able to resume their normal lives, including playing recreational sports.
"People often find that they can function better after surgery because they no longer experience pain every time they move," Phillips says.
3. Fusion shouldn't be the first treatment option …
According to Phillips, surgery is almost always considered only after a conservative approach — physical therapy, spinal injections and/or medications — fails to alleviate symptoms.
"I rarely, if ever, recommend having surgery without first trying nonsurgical options," he says. "However, if conservative measures aren't working, you shouldn't stick with them indefinitely. There's no benefit to going through months or even years of injections if you're still experiencing back or neck pain, or numbness or tingling in your legs."
4. … But it is sometimes the best option.
An NIH-funded study conducted at Rush and 10 other sites nationwide showed that patients suffering from degenerative spondylolisthesis with spinal stenosis who underwent fusion surgery experienced substantially greater pain relief and improvement in function over four years than patients who were treated nonsurgically.
Fusion has also proven to be a highly effective treatment for spinal instability or deformity.
"We've been able to show that in appropriate patients, we can achieve excellent outcomes with fusion," says Phillips. "But it's important to be evaluated by a qualified spine surgeon who can determine the best course of treatment based on your specific condition."
I rarely, if ever, recommend having surgery without first trying nonsurgical options. However, if conservative measures aren't working, you shouldn't stick with them indefinitely.
5. Fusion can't heal the whole spine.
Once a fusion heals, the level or levels that have been fused should not cause further pain or require further treatment down the road.
But Phillips cautions that if the underlying problem is arthritis, other levels of the spine can be affected and wear out over time.
"Fusion is not a fix for the entire spine; we can't change the natural progression of arthritis in other areas of the spine," he says. "The good news is that we can surgically address specific areas of damage and effectively alleviate symptoms."