The last decade has seen many life-changing medical breakthroughs — from a cure for hepatitis C to the world's first artificial pancreas for people with diabetes.
What might tomorrow bring? Here’s a look at current trends — and the ways they might change the future of medicine.
Treating cancer with genetic data
Since the 1950s, chemotherapy has been one of the most successful treatments for cancer. In some cases it can cure the disease, and it helps many other people enjoy long-term remissions even if it doesn’t make them cancer-free.
As with any medication, chemotherapy drugs can cause side effects. That's largely because most chemo medications, as they travel through the body, attack fast-growing healthy cells — in areas like the mouth and digestive tract and in hair follicles — as well as fast-growing cancer cells.
One recent advance that is helping patients live longer — and may spare them some of the side effects of traditional chemotherapy — is targeted treatments.
Unlike standard chemotherapy drugs, targeted medications zero in on the specific genetic changes in cancer cells that make them different from normal cells. This precise focus on cancer means the drugs usually don't harm healthy cells.
Targeted therapy is already approved for certain kinds of cancer, such as melanoma and some types of leukemia and lung cancer. But it is not comprehensive because it's currently limited in the types of cancer it can treat.
Cancer specialists at Rush and around the country hope to change that in the near future. They're working with Chicago-based Tempus to create a database of patients with similar genetic profiles, along with the targeted treatments that work for them. That information might one day allow doctors to use targeted drugs to treat anyone with cancer.
Rush also participates in the National Cancer Institute's Match trial. In this ongoing nationwide study, patients are tested to determine the genetic makeup of their tumors. If their tumors have genetic changes that match one of the targeted therapies available in the trial, the patient may receive that treatment.
The results of the Match trial will help establish whether targeted therapies will be effective for people whose tumors have specific gene mutations — regardless of their cancer type.
The goal with both Tempus and Match is to treat the genetic changes that are the underlying cause of the cancer.
"The characterization of the genetic background of cancer and analysis of patient response to treatment will be at the heart of our clinical and research efforts at Rush,” said Ranga Krishnan, MB, ChB, an internationally renowned researcher and CEO of the Rush University System for Health. "This will allow us not only to identify pathways to more personalized treatment, but also to discover novel biomarkers for early diagnosis and treatment."
The goal ... is to treat the genetic changes that are the underlying cause of the cancer.
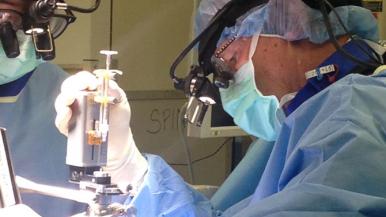
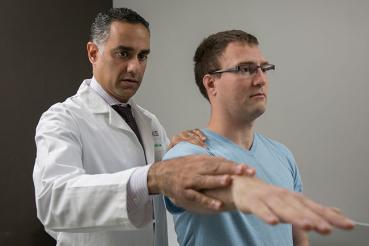
Reversing paralysis
An experimental treatment is helping people with certain paralyzing spinal cord injuries regain some movement in their hands and arms.
Neurospine surgeon Richard Fessler, MD, PhD, and his research team at Rush recently gave progressively larger injections of embryonic-derived stem cells to a small group of people with partial spinal cord tears who are paralyzed from the neck down.
After receiving the treatments, three of the five participants regained the use of their hands and arms. They could feed, wash and partially dress themselves, for instance.
"We have not cured paralysis, but we have moved it from it being untreatable to partially treatable," he says.
In spinal cord injuries, some neurons are completely destroyed. But others may simply have lost the protective coating (myelin) that allows them to function. "What we think is happening is these stem cells are creating myelin and recoating the potentially functional cells," Fessler says.
He envisions a day when frozen stem cells will be stored at hospitals in case someone arrives with a spinal cord injury.
Younger patients, faster recoveries for knee replacements
Doctors used to encourage people to wait until at least age 65 to have knee replacement surgery. The reason? Implants lasted only about 10 years.
But today's prosthetics are made to function longer — many artificial knee joints last at least 20 years before they need to be replaced. This makes knee replacements a more viable option for people in their 50s.
Younger adults increasingly need knee replacements because of severe arthritis, often a result of their active lifestyles, says Denis Nam, MD, MSc, a joint replacement surgeon at Rush who specializes in hip replacement and knee replacement.
Obesity is another reason why younger people are seeking new knees.
"Both trends — more active people and more obese people — will most likely mean more knee replacements because of the amount of stress they're putting on their knees," Nam says.
Another trend in knee replacements that is expected to continue: outpatient surgery.
"A lot of people who have a knee replaced can literally go home the same day as their surgery," Nam says. "Not all patients are candidates for this, of course. But it's projected that almost 20 percent of knee replacements — and other types of joint replacement — will be done on an outpatient basis by 2020."
For patients who do require a hospital stay for a new knee, the emphasis at Rush is on a speedy recovery and quick discharge. "Almost all hospitalized patients are walking the day of surgery, and they're in the hospital for one night, maybe two," Nam says. It wasn't all that long ago — in the 90s — that knee replacement patients spent a week or more in the hospital.
"We've learned a lot over the years — and will continue to learn — about how to safely do knee replacements in a wider spectrum of patients and how to make their recovery faster so they can get back to their lives much more quickly."
Considering joint replacement surgery?
Rush has one of the world's top joint replacement programs, and surgeons at Rush replace more than 3,800 hips and knees every year.
You may be able to participate in a clinical trial.
Learn more about the many clinical trials for cancer available at Rush.